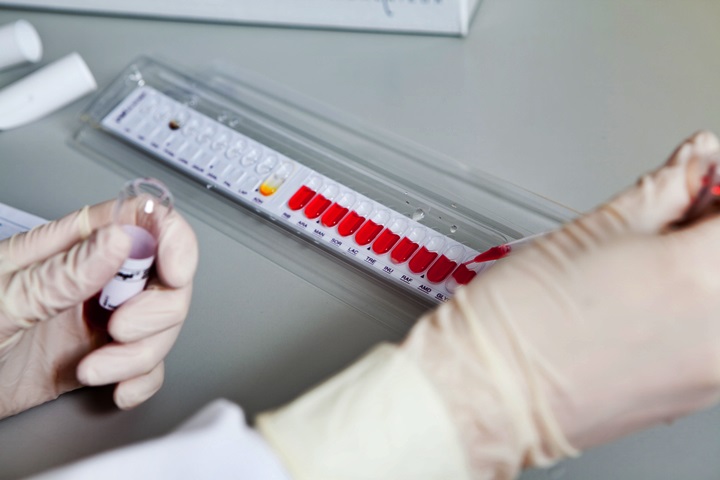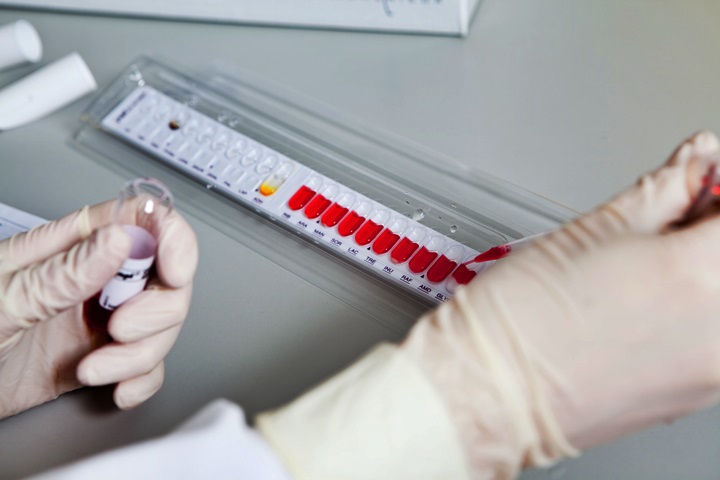
After you have made the decision to store your child’s umbilical cord blood, you are given the option to have HLA tissue typing performed on the blood. This test is performed to help assess the compatibility of the stem cells with potential recipients. This kind of test is very important if you believe that the stem cells may be used by someone other than the child they came from.
What is HLA?
Human leukocyte antigens (HLA) are proteins found on cells within the human body. HLA proteins are also referred to as a marker. Scientists have already identified more than 2,500 different HLA markers. Each HLA marker is identified by a letters and/or numbers.
Human leukocyte antigens help the body tell the difference between normal tissue and foreign objects. If foreign tissue is injected into the body with vastly different HLA, it can be rejected by the immune system, a condition known as graft versus host disease (DVHD).
HLA markers are inherited from parents, with 50% from your mother and 50% from your father. Because of the randomness of markers inherited by children from their parents, siblings only has a 25% chance of being compatible.
One of the reasons why parents tend to store the umbilical cord stem cells for each of their children is because of the risk that siblings may not be compatible.
______________
Learn more about storing your baby’s cord blood at birth:
Public & Private Cord Blood Banking: Pros & Cons
Simple Steps to Cord Blood Banking for Expectant Parents
4 Cord Blood Banking Myths and Misconceptions for Expectant Parents
______________
What is HLA Tissue Typing?
The test simply records the types of HLA present within an umbilical cord blood sample. Performing HLA tissue typing prior to freezing umbilical cord blood gives parents more information about the potential compatibility of the stored cord blood sample. If the test is not performed on the umbilical cord blood sample, it must be performed at a later date on the donor or on a portion of the frozen sample
Assessing compatibility
When assessing compatibility between donor and recipient, two main groups of human leukocyte antigens are used. The first group has three classes of antigens (HLA-A, HLA-B, HLA-C) and the second group has one class (HLA-D). The first group of antigens is commonly found on blood cells, the second group is only found on certain types of tissue.
For a stem cell sample to be considered compatible, a doctor will need to match at least 6 of 8 HLAs reviewed. 8 are considered the minimum number of HLAs to review. Because umbilical cord stem cells are less mature, between 4-6 markers spread across the HLA-A, HLA-B and HLA-D classes must be a match.
The tests can be quite complex and vary depending upon the type of transplant to be performed as well as the tissue being used.
Cells4Life use a very comprehensive level of detail when testing which human leukocyte antigens are present in an umbilical cord blood sample, so doctors can easily assess compatibility.
Transplants can sometimes succeed despite only having a partial HLA match. Umbilical cord stem cells are more likely to succeed than adult cells in a partial match transplant. This is because the cells are less mature and less likely to trigger an immune system response.
To learn more about HLA tissue typing, please contact us today!